Last winter, 32-year-old Samantha Patterson got sick with COVID-19 and, like so many, struggled to recover.
She had lingering symptoms, including chest inflammation, up to six months after she cleared the virus. She said she took the vaccine as soon as it was available to her because she knew it was possible to become infected with COVID again, despite developing antibodies against it.
A resident of Southern Pines, Patterson was working in a skilled nursing facility in Fayetteville, North Carolina when COVID-19 first appeared. From the start of the pandemic, she was as safe as possible to protect herself and the lives of the elderly residents she worked with.
“I was constantly wearing masks at work, I wasn’t going out and socializing or seeing family,” she said. “I didn’t even go to the grocery store. I feel extremely responsible for the lives of the older adults I work with, so I was as careful as you could possibly be. Then, one Friday in early Dec., I got a tickle in my throat.”
The itch in her throat escalated to a plethora of symptoms known to accompany the virus: headache, fatigue, chills, fever, dry cough. She drove to a rapid testing center and within 30 minutes received a positive result. Patterson said the more her symptoms worsened, the more fearful she became of possible hospitalization and ventilation. She had what her doctor described as “breath hunger.”
“I’m young and healthy, with no preexisting health conditions,” she said. “I exercise frequently and regularly run miles and have good lung capacity, but with COVID I always felt like I couldn’t breathe. Every moment of the day and night, I lived in fear that I wouldn’t be able to breathe.”
Patterson said she became so sick she could not stand without passing out. Eventually, she got a ride to the emergency room at FirstHealth Moore Regional Hospital, where doctors performed a chest X-ray that came back clear. “I still had chest inflammation, but it did give me peace of mind to know my lungs were not full of fluid, which is what it felt like,” she said.
After receiving an IV of fluids, she was sent home with instructions to drink Pedialyte® instead of water. She was told her fever was burning off the gallons of water she was drinking, leaving her dehydrated and depleted of electrolytes.
“I was also prescribed an anti-anxiety medication that I took once a day because I was essentially in a state of panic all the time, not knowing if I was able to effectively breathe or not. I barely remember those two weeks. No systems in my body were working properly,” Patterson said.
The storm broke around day nine and she started to feel slightly better. Short walks still left her out of breath and quickly exhausted, but at least she could walk. After a full quarantine and negative tests, Patterson went back to work but continued to experience lingering symptoms. For about five or six months, she said she had sporadic feelings of pain in her face and drinking anything cold was uncomfortable.
There were also cycles of chest inflammation that would last about five days at a time. Her primary care physician ordered an echocardiogram to ensure there was not any permanent damage to her heart. The test revealed no lasting heart damage and the bouts of chest inflammation gradually disappeared, although Patterson said she gave up her morning coffee for a few months after realizing it contributed to the chest pain.
Patterson took the vaccine as soon as her place of work made it available to staff in Jan. of 2021. She said she looked over the research on the vaccine, read about the methods researchers chose, and ultimately decided to listen to the experts.
“I understand the hesitancy around the vaccine, but not getting vaccinated was so much scarier to me,” she said. “Especially since COVID also took a huge toll on my mental health. Not only from the isolation, but I do think it changed something in me chemically. I eventually got my mental health under control, but I absolutely do not want to go through that again.”
Patterson said since being vaccinated she has enjoyed being able to reengage in her life and do things like go to the gym and meet her sister’s newborn without putting anyone at risk.
If you would like to get vaccinated, FirstHealth is offering COVID-19 vaccines at several of its primary care and occupational health clinics in its service areas. Call (910) 715-7468 to schedule an appointment or visit www.firsthealth.org/shot to learn more. To check vaccine availability at the Moore County Health Department call (910) 947-7468. For the Richmond County Health Department, call (910) 417-4909.
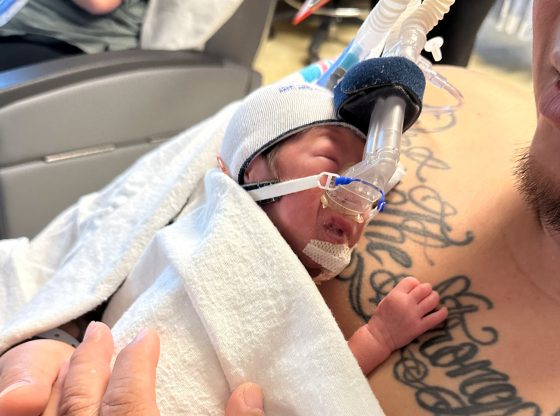
Photo: Samantha Patterson and her son, Miles. Courtesy photo.
Contributed